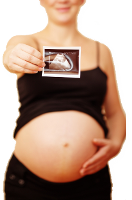
Postpartum Pointers
Getting Through Those First Weeks at Home
| Share: | Tweet | Thank You! |
Physical
Episiotomy & Stitches: Your body has been through a lot. If you were able to deliver vaginally you may have had an episiotomy or suffered torn muscles between the base of the vagina and the rectum. Repaired with dissolving stiches, these injuries can take several weeks to heal completely. Often the source of great bathroom anxieties - stitches are one of the most common complications that leave many women wishing they could avoid a bowel movement all together. Stool softeners and a diet that is high in fiber and liquids can help make that first bathroom break a bit more bearable. Just remember to take your time and don't strain if you can avoid it. Most women find that it isn't as bad as they thought it would be.It is important to keep your episiotomy or repair clean by using your sitz bath or cleansing gently in the shower. Keep an eye out for signs of infection and make sure to report any foul smelling drainage, swelling, or worsening pain from your stitches to your doctor.
Hemorrhoids: If you are one of the lucky few women who made it through your pregnancy without a hemorrhoid or two you may be wondering how they could appear after delivery. Often developing with the pressure of pushing, you may have these engorged veins to some degree for the rest of your life without any major problems. Itching, soreness, pain and occasional bleeding can happen with hemorrhoids, and it usually isn't a problem - but make sure to point them out to your doctor when you return for your follow up appointment.
Follow Up Appointments: Follow up appointments for vaginal deliveries are usually at around 6 weeks. C-sections can expect a trip back to the office in one to two weeks, unless you have a problem that requires you be seen sooner. Your doctor will be talking with you about birth control at this visit, so if you haven't given it much thought yet, do so before your appointment. Remember - no sex for four to six weeks after delivery (yes, you too C-sections) so that your pelvic muscles and vagina can heal properly. And, not to mention, that you are probably not going to be on any birth control and any act of sex could potentially have you in a motherly way again before you can say "month old baby". Yikes!
Cesarean Section: If you have delivered by Cesarean section, your biggest challenge is going to be overcoming pain and working to regain your mobility and independence. You will probably not be allowed to lift anything heavier than the baby, and it can be very stressful for moms to manage daily activities - especially if there are younger children in the home. Do your best to pace yourself and rely on others for help. Walking will help you relieve some of the soreness in your abdomen, but don't overdo it. If you have staples or stitches, your doctor will want to see you back in the office usually within one to two weeks to have those removed. Watch your incision (or have someone else watch it if you can't see it) for discharge, foul odor, or new redness and report this to your doctor. Your bleeding may be lighter than that of a vaginal delivery - lasting only a week or two, but remember that you have had major surgery so keep your activities light. Because your risk for a blood clot is higher after a C-section, make sure to contact your doctor if one leg swells, has new pain, gets red, or feels hot.
Bleeding: Vaginal bleeding will continue in some women for up to six weeks. For a few, it can be only two or three weeks, but every woman will have bright red bleeding at first, followed by brown and eventually a white discharge. Known as lochia, this discharge has a somewhat different smell than your regular period, but should never smell bad. Any foul smelling blood or bleeding that gets suddenly heavier to the point you are saturating a pad an hour should be evaluated by your doctor as soon as possible. It is normal to pass a small clot (the size of a quarter or less) or two after you get home, but report to your doctor if you pass any large clots (softball size) or a pile of small clots.
Breasts: Breast changes can be one of the most dramatic for the postpartum mom. If you have chosen to breast feed, your breasts will begin to get hotter, heavier and possibly leak as your true milk comes in - usually about 48-72 hours after delivery. If your baby isn't latching well, or isn't emptying the breast properly, some women may develop engorgement as a result. This painful over-filling of the breasts with milk can feel like you are carrying two rock-hard boulders on your chest. Some women may give up nursing all together because of it, but there's no need. If you get engorged you may also run a fever. Taking anti-inflammatory medications like acetaminophen or ibuprofen as directed is fine when nursing and heat may be applied as needed. If your breasts become too hard for baby to latch, you may express just enough milk to soften the nipple. Engorgement usually disappears on its own with a few days.
Bottle feeding moms may also experience engorgement on postpartum day 4 or 5. Keep your breasts well-supported in a tight bra and do your best not to stimulate them. Shower with your back to the water and even though you may want to express milk for some relief, don't do it. Whatever you release triggers your body to make more.
Another common breast complication is from infection known as mastitis. Mastitis can cause one or both breasts to be hard, hot, and swollen, and may have red streaks running up from the nipple onto the chest. Fever is also another indication of a breast infection and any of these symptoms should be reported to your doctor right away. It is still acceptable to continue nursing if you should develop mastitis.
Mental
Shifting hormones can make those first few days home with baby full of ups-and-downs. You may find yourself crying at commercials on television - or maybe you are laughing and crying at the same time, but having no idea why you are doing either one. These normal swings are known as the baby blues. For some women they can start as soon as 24 hours after birth and can be expected to last about a week before they begin to taper off. Any mood swings or sadness that last longer than one to two weeks and is accompanied by more severe symptoms could be postpartum depression.Postpartum depression affects approximately 25% of all women either mildly or with more serious symptoms. Women at the highest risk for developing postpartum depression can include moms without a good support system, women with financial struggles, or a history of depression in the past.
Symptoms of PPD include:
- Sleeping too much or too little
- Not wanting to care for your baby
- Crying uncontrollably for no reason
- Anxiety and nervousness
- Thoughts of hurting yourself or your baby
- Fatigue
- Thoughts of worthlessness
Most cases of PPD respond quickly to antidepressant medications and after a short treatment, most moms are able to stop the medications without any further problems. If you have suffered from depression in a previous pregnancy there is a greater chance you may suffer from it with subsequent pregnancies. Just make sure to talk with your doctor and have a game plan in place so that you can be prepared should you need to face round two.
And above all - you must stay safe. If you have any thoughts of hurting yourself or your baby, find a trusted friend or health care provider that you can talk to. Being honest is the only way to get the help you need so you can focus on caring for your baby.
Welcoming a new baby to the family is a wonderful event. While there will be plenty of sleepless nights, lots of adjusting and maybe even a little bit of worry, these are the best days. Remember to take care of your family by first taking care of yourself.
| Share: | Tweet | Thank You! |

 Community
Community